Living With Eczema That Won’t Go Away: What to Do When Treatments Stop Working
February 11, 2026Few skin conditions are as stubborn and misunderstood as hidradenitis suppurativa (HS). Despite advances in medicine, even the most promising treatments often provide only fleeting relief. The reason? HS is driven by a tangled web of immune signals, making it one of the most challenging inflammatory diseases to manage.
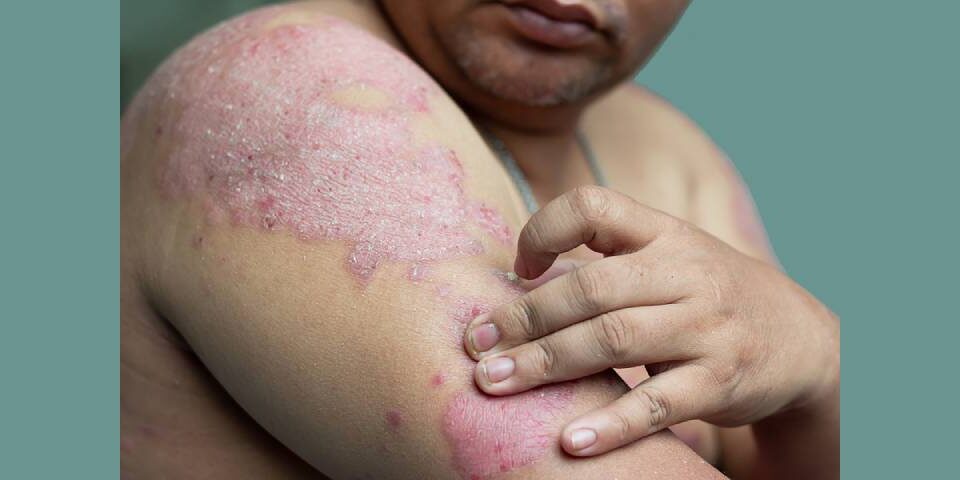
For those affected by HS, the impact goes far beyond the skin. Painful, red nodules often develop in sensitive areas like the inner thighs, armpits, buttocks, groin, and under the breasts—bringing not only physical discomfort but also emotional distress. Many individuals try multiple treatments, only to see symptoms return.
But new possibilities are emerging. At Apex Clinical Research Center, ongoing HS clinical trials are focused on targeting the underlying immune mechanisms of HS, with the goal of developing longer-lasting relief and new hope for patients.
Hidradenitis Suppurativa Is an Immune-Mediated Inflammatory Disease
One of the reasons treatments for hidradenitis suppurativa are so challenging is that HS is a biologically complex, immune-mediated disease. It’s not simply an infection. It’s not about cleaning out clogged pores or better hygiene. The agonizing nodules are the body’s inflammatory response to the immune system attacking its very own hair follicles.
Dermatology research has revealed that this dysregulated immune response centers around three key inflammatory pathways:
- TNF-alpha: Also called “tumor necrosis factor,” the activity and amount of these pro-inflammatory cytokines in the system seem to play a role in aggravating nodule formation in HS patients.
- IL-17: Interleukins IL-17A and IL-17F are also inflammatory cytokines implicated in the development of hidradenitis suppurativa.
- IL-1: Interleukin IL-1 is another inflammatory cytokine that seems to become dysregulated in patients with HS.
Because HS attacks through multiple dysregulated immune pathways simultaneously, it is fundamentally challenging to control in the long term with current hidradenitis suppurativa treatment options. As dermatology research has advanced, however, hidradenitis suppurativa clinical trials have found promising potential treatments that inhibit or block multiple cytokines at once, and these in particular. This new approach may reduce the inflammatory immune responses that HS patients struggle with, providing more reliable relief.
The Self-Perpetuating Cycle of Inflammation in Hidradenitis Suppurativa
Because of the multiple inflammatory immune actors converging at the same time within the bodies of HS patients, the manifestations of the disease can spiral into a seemingly never-ending cycle of distress. Interrupting and ultimately preventing the inflammatory cycle that includes these issues makes the need for ongoing dermatology clinical trials focused on HS all the more urgent:
Immune Activation
People with hidradenitis suppurativa experience an abnormal activation of the immune system that, instead of defending the body against an actual pathogenic invader, turns its inflammatory attack inward, onto its own hair follicles. Dermatology research indicates that between 77% and 80% of HS patients have a genetic disposition toward the disease. Although the precise genes responsible for the disease have yet to be discovered, there is some link between the genetic makeup of people who have HS, Crohn’s disease, and other rare inflammatory conditions. Environmental factors like stress, sweat, obesity, friction, smoking, and infections may also cause the affected genes to trigger this dysregulated immune activation.
Follicle blockage and rupture
An HS-caused immune system attack on the hair follicles severely plugs them, causing the growth of painful, pea-sized nodules under the skin—significantly larger than the follicles themselves. This painful pressure can eventually rupture the affected follicles.
Abscess formation
The resulting abscesses fill with foul-smelling pus that can burst open and drain, causing both pain and emotional distress and embarrassment. HS abscesses can also be prone to infection, which can aggravate the situation further.
Sinus tracts and scarring
In more advanced cases, HS abscesses can also form tunnels under the skin called sinus tracts between each other underneath the skin’s surface. Both the abscesses and the tunnels can cause intense scarring, additional complications, and infections.
Why HS Can Become Progressive Over Time
In the early stages of HS, it can be mistaken for other conditions, such as severe acne. Therefore, most patients do not receive an official hidradenitis suppurativa diagnosis and subsequent treatment until they reach the point of sinus tract scarring. During that time, HS flare-ups can reach deeper below the skin’s surface, affecting even the fascia, muscles, and lymph nodes.
These complications can severely impact a person’s quality of life, physically and emotionally. In fact, research shows that patients with HS are about 50% to 70% more likely to struggle with depression and anxiety because of the condition. This additional stress can trigger additional immune system dysregulation events, which can worsen HS further. This adds to the urgency for HS clinical trials.
Why Standard Hidradenitis Suppurativa Treatment Options Don’t Work for Everyone
Currently, there is no cure for HS, but there are several treatment options that can address symptoms and provide some comfort, at least temporarily. For many patients, however, current treatments only bring diminishing returns or stop working altogether—a cycle that can be both physically and emotionally exhausting. Some of the primary issues with current HS treatments that our dermatology clinical trials for hidradenitis suppurativa are trying to solve include:
Antibiotics
Your dermatologist may prescribe antibiotics for HS, not specifically for infection, but to reduce the inflammatory response. This is only a temporary measure, as patients cannot remain on an antibiotic for more than two or three months at a time without side effects. Also, an antibiotic cannot calm and block all of the different inflammatory cytokines firing at once to stop attacks on the hair follicles.
Biologics
Biologics are promising medications that can target specific immune-mediated pathways for HS. However, since HS involves multiple immune drivers at the same time, one biologic medication that targets one driver may not affect the damage caused by the other drivers.
Hormonal and Genetic Variability
The complex genetic and hormonal landscape between HS patients poses another formidable challenge to the successful, long-term treatment of hidradenitis suppurativa. The more data we can collect about these variables during HS clinical trials, the more we can understand how these factors impact disease manifestations, thereby opening up new pathways for more individualized, targeted, and successful approaches to hidradenitis suppurativa treatment.
Differences in Disease Severity
Of course, any level of HS is severe enough to warrant seeking relief, but the differences in severity between mild, moderate, and severe also pose problems in finding effective treatment. This is especially true for milder cases that patients may not understand at first, and which clinicians may not initially diagnose correctly. Our dermatology clinical trials are also concerned with developing better ways to diagnose the earlier stages of HS so that effective treatment can begin sooner.
Treatment Response is Highly Individualized
Even patients with seemingly similar courses of hidradenitis suppurativa can have completely different responses to treatments. Our HS clinical trials also seek to uncover some of the mechanisms behind why individual patients react differently to the same treatment, so that future treatments can also be more individualized.
Advancing Hidradenitis Suppurativa Treatment Through Targeted Research
Apex Clinical Research Center is currently enrolling adolescents and adults in a Phase 2–3 clinical trial for hidradenitis suppurativa to address these gaps in understanding and treatment, so we can discover and develop better, earlier interventions for HS. This study is evaluating investigational topical, oral, or injectable therapies designed to reduce painful lesions and combat the underlying inflammation that causes them. Our hidradenitis suppurativa clinical trials may be appropriate for individuals experiencing the following HS symptoms:
- Multiple active or draining HS lesions
- Symptoms that have been present for six months or longer
- Inadequate symptom relief from current prescription treatments
Participating in our HS clinical trials could be the piece of the puzzle you’ve been looking for in finding hidradenitis suppurativa relief for you and other fellow patients. All study-related care is free, and compensation is available for time and travel costs. Your participation is voluntary at all stages, and we will closely monitor your safety and all aspects of your medical condition throughout the study. We can then pass on the information we gather to your healthcare providers, so they can better guide your ongoing care regimen in the future.
If you have any questions about participating in our HS clinical trials, please contact us today. We are happy to answer all of your questions and make sure you can make informed decisions about participating. We also have flexible scheduling options at our Canton and Mayfield Heights locations.
Shape the Future of Hidradenitis Suppurativa Treatment: Participate in Our HS Clinical Trials
Hidradenitis suppurativa is a difficult and complex autoinflammatory condition to treat, no matter how dedicated you’ve been to your treatment regimen. Setbacks do not reflect personal failures. Fortunately, ongoing research into the cutting-edge treatment of hidradenitis suppurativa is expanding your options and discovering more pathways to relief every day. We invite and encourage patients with moderate to severe HS to contact the Apex Clinical Research Center team today to learn more about participating in hidradenitis suppurativa clinical trials.